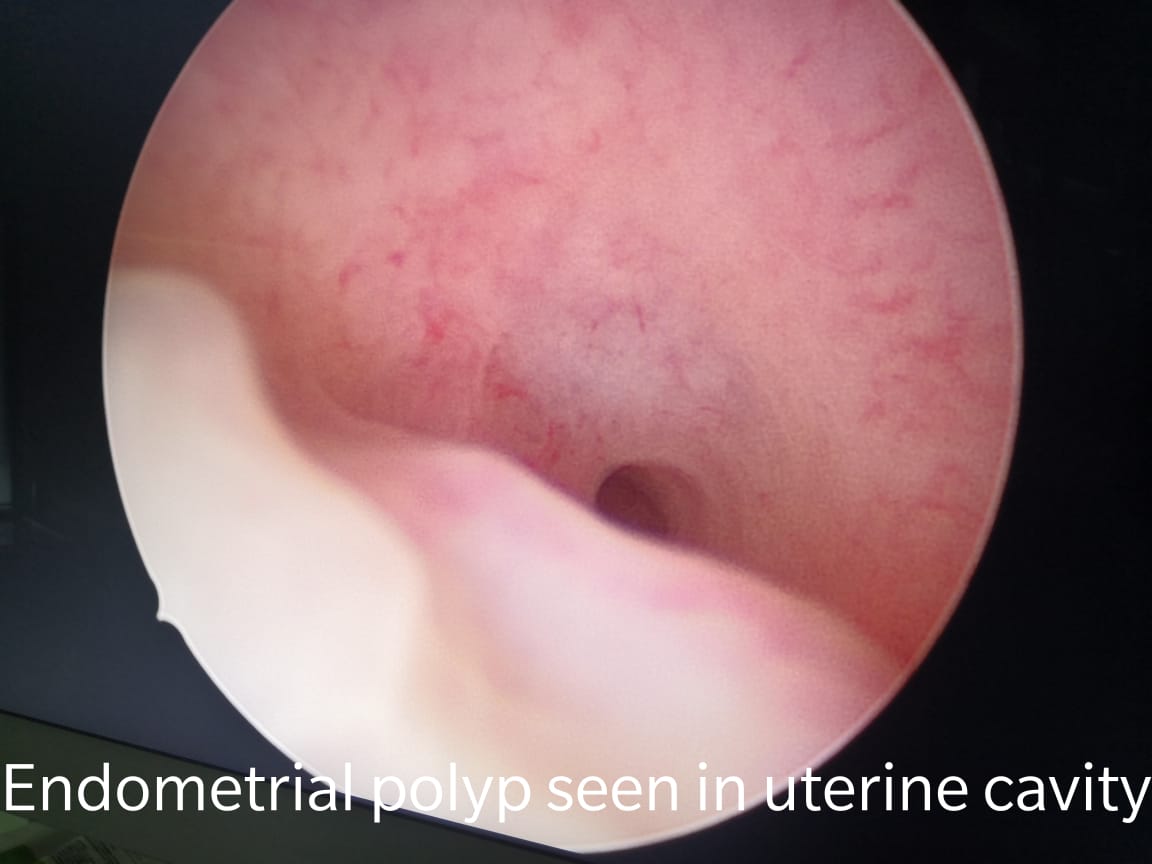
Uterine or endometrial polyps are growths attached to the inner wall of the uterus that extend into the uterine cavity. Overgrowth of cells in the lining of the uterus (endometrium) leads to the formation of ensdometrial polyps, also known as uterine polyps. These polyps are usually noncancerous (benign), although some can be cancerous or can eventually turn into cancer. They can range from few millimetres to few centimeters and can be endometrial, endocervical or cervical polyps depending on the origin of the tissue.
Symptoms
Signs and symptoms of uterine polyps include:
- Irregular menstrual bleeding — for example, having continuous, unpredictable periods of variable length and heaviness
- Bleeding between 2 menstrual periods
- Excessively heavy menstrual periods
- Vaginal bleeding after menopause
- Infertility
Some women have only light bleeding or spotting; others are without symptoms.
Causes
Doctors don’t know exactly why women get uterine polyps, but it may be related to changes in hormone levels. Each month, your estrogen levels rise and fall, directing the lining of the uterus to thicken and then shed during your period. It’s an overgrowth of that uterine lining that makes a polyp.
Some things make you more likely to have polyps. One is age ,they’re more common in your 40s or 50s. That may be due to the changes in estrogen levels that happen right before and during your menopause.
Obesity, high blood pressure and taking the breast cancer drug tamoxifene can also raise your chances for uterine polyps.
Diagnosis
Transvaginal ultrasound
Hysteroscopy
Endometrial biopsy
Treatment modalities
Watch and wait
Medication :Some studies have shown polyps less than 5 mm can be treated with course of progesterones for upto 3 cycles, polys might regress or be she’d out in next menstrual cycle.
Hysteroscopy:
Hysteroscopy had been accepted as the gold standard in diagnosis and treatment of all types of polyps. It is usually done as a daycare procedure and the obtained tissue is sent for histopathology diagnosis.
What to expect with hysteroscopic removal of endometrial polyp
Prior to surgery
- You may be asked to stop taking aspirin, ibuprofen (Advil, Motrin), naproxen (Aleve, Naprosyn), Clopidogrel (Plavix), warfarin (Coumadin), and other blood thinners.
- You will be scheduled to undergo the procedure after menstrual bleeding has ended and before ovulation (if you are still ovulating).
- Ask your doctor which drugs you should still take on the day of the surgery.
- Discuss any possible bleeding disorders or other medical conditions that you may have.
- You will have blood samples taken in case you need a blood transfusion.
- Do not smoke. This will help you to recover quicker.
On the Day of the Surgery
- If you are to have general anesthesia, you will usually be asked not to drink or eat anything after midnight the night before the surgery.
- Take the drugs your doctor told you to take with a small sip of water.
- Your doctor or nurse will tell you when to arrive at the hospital.
After Surgery
- Most patients can go home the same day.
- You may have increased cramping and vaginal bleeding for a day or two after the procedure.
- You may experience gas pains for about a day or so due to gas administered during the procedure. This may extend into your upper abdomen and shoulder. Walking will help relieve this pressure.
- This surgery has a quick recovery with most patients feeling much better within the first few days.
Recovery: what to expect in the next few weeks
- Some women have some water discharge with some blood for a few weeks expect the flow to be heavy at first and then diminishing over time.
- Most women feel better within the first week following surgery; however, do not lift, push or pull any heavy objects for a couple of weeks.
- Do not resume sexual intercourse or douche until your doctor says it is OK.
- Full recovery takes about two weeks to allow for internal healing.
Dr.Ruchi Tandon is a trained hysteroscopic surgeon with over 13 years of clinical experience. At present, she is providing her services in leading hospitals in South Delhi namely, Apollo Spectra, Apollo Cradle Royale and Max Smart super speciality hospital, Saket.