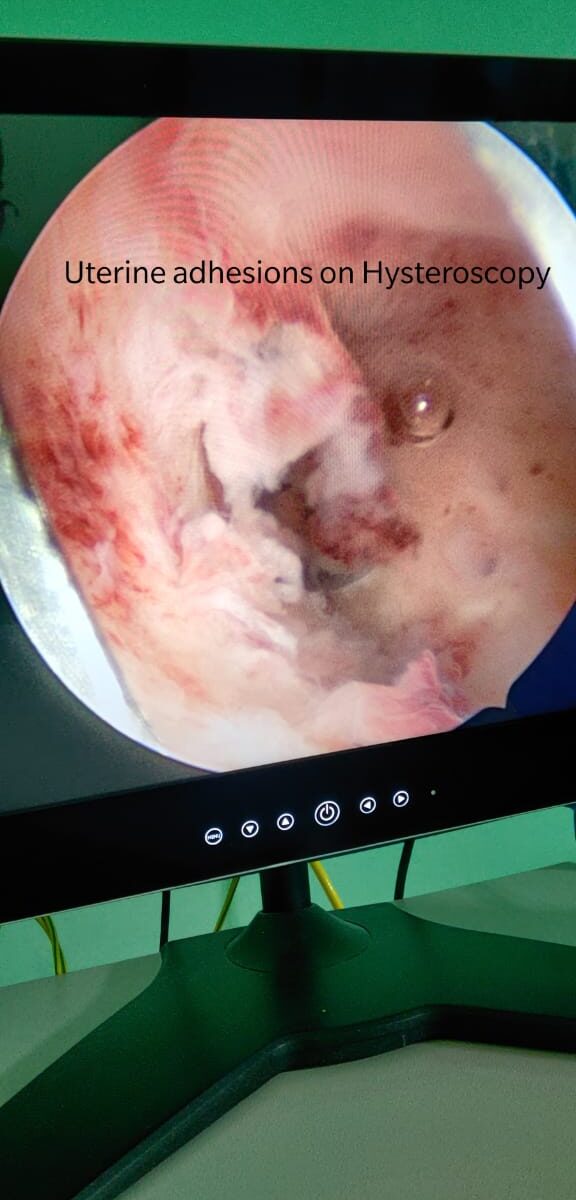
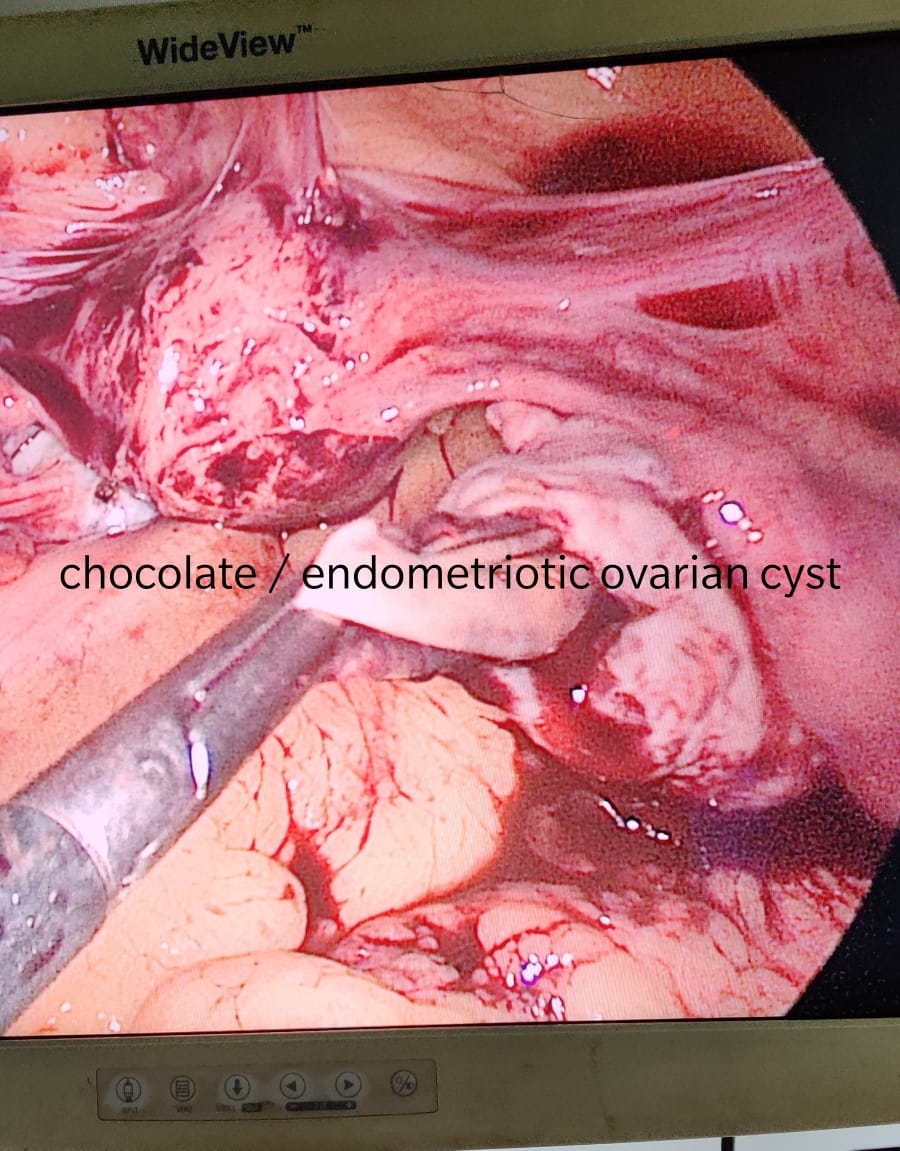
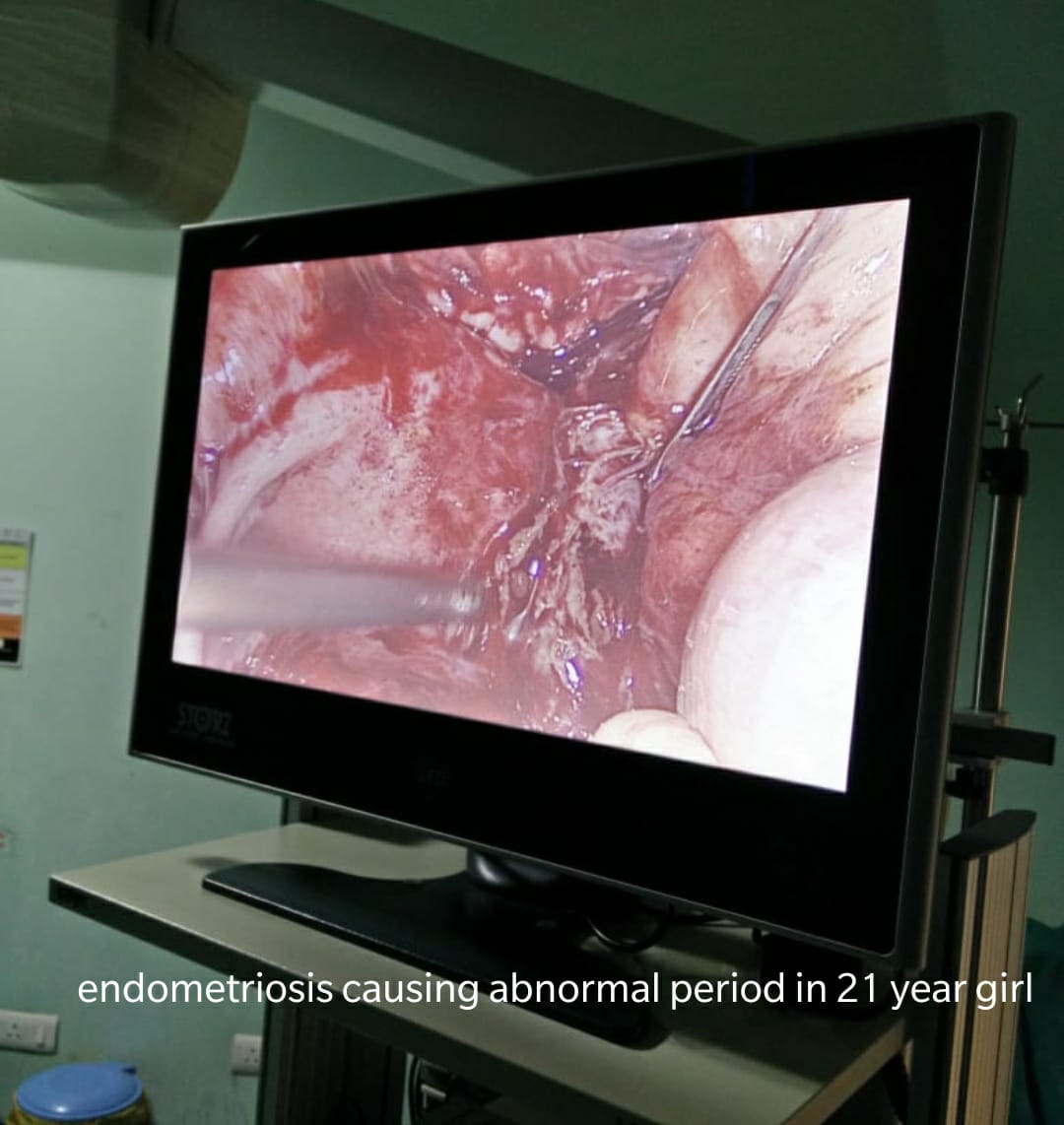
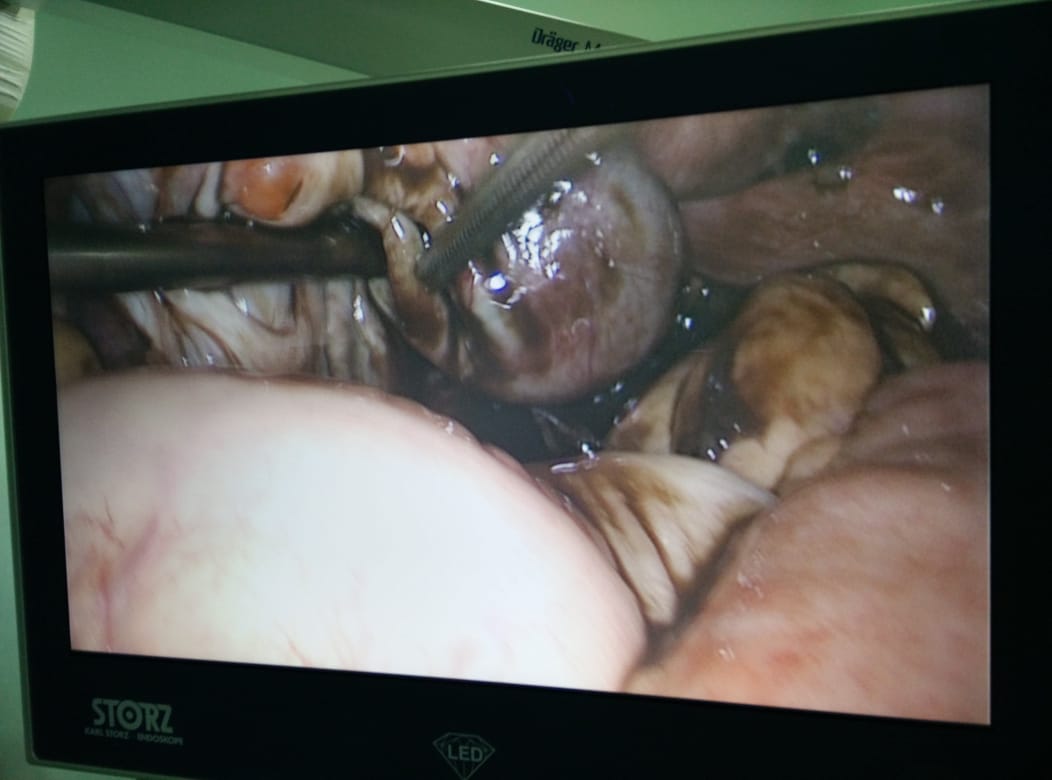
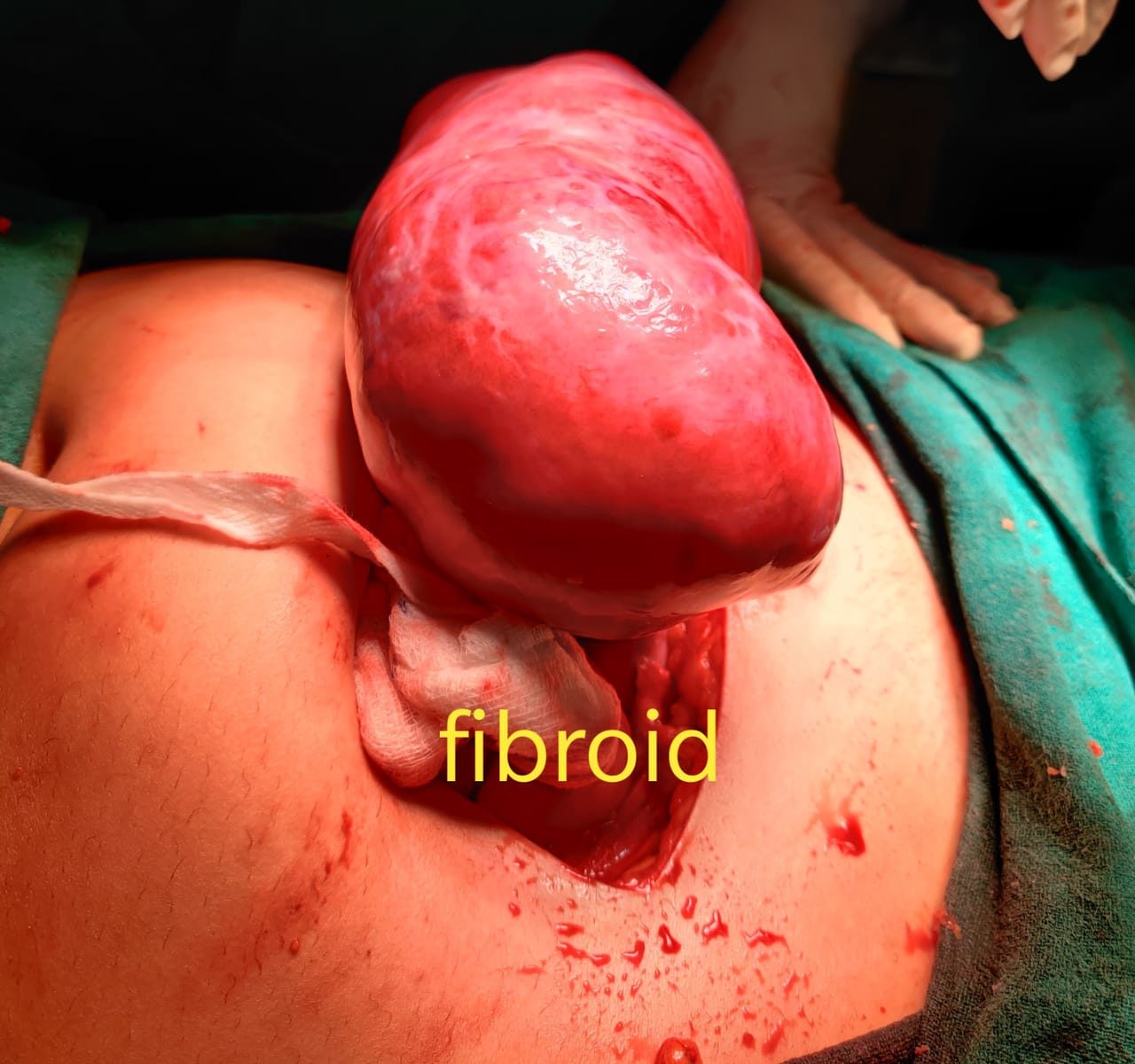
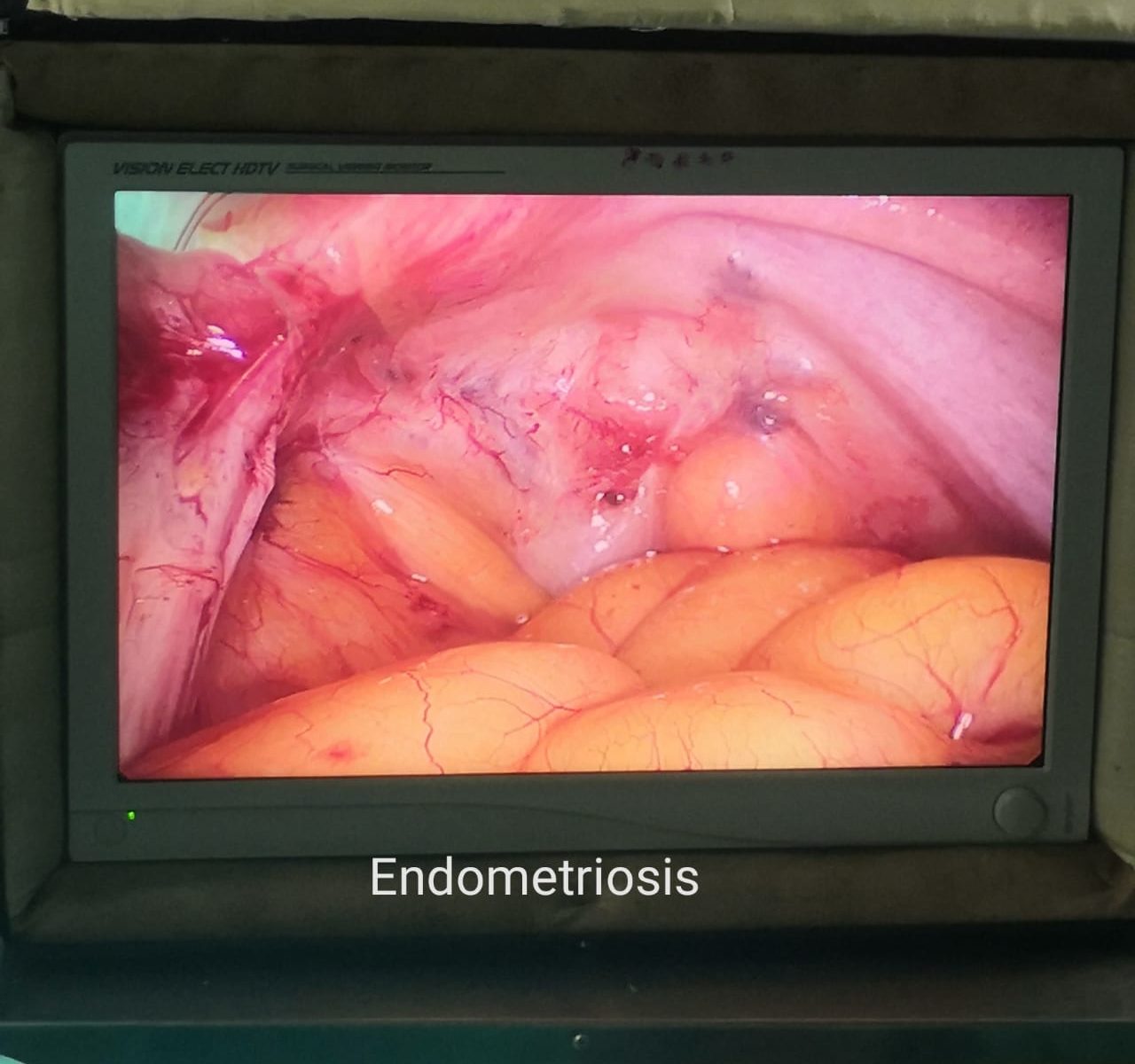
Pelvic adhesions, sometimes referred to as “scar tissue”, are a common cause of both infertility and pelvic pain.
Pelvic adhesions can occur as a result of a variety of different conditions including endometriosis, pelvic infection, and previous abdominal or pelvic surgery. It is well known that pelvic adhesions develop over 90% of the time following major abdominal surgery. The most common types of surgery that predispose to the development of pelvic adhesions include the removal of uterine fibroids (myomectomy), treatment of endometriosis, removal of ovarian cysts, and the repair of obstructed fallopian tubes.
Many complications can occur as a result of pelvic adhesions. For example, it is thought that adhesions may be a significant factor in as much as 40% of cases of infertility. They are also thought to be responsible for up to 50% of cases of chronic pelvic pain. In addition, adhesions are typically responsible for 50-75% of cases of bowel obstruction. Although more recent data are lacking, the treatment of pelvic adhesions accounted for 3% of all surgical procedures performed in the United States in 1998, as well as 1% of all hospital admissions and 2% of all patients admitted for surgeries around that time.
How do pelvic adhesions occur?
Adhesions typically develop in response to injury, as part of the normal healing process. Immediately following injury, cells that cause healing (inflammatory cells) migrate to the site of the injury. Within seven days following injury, the scaffold for healing or adhesion formation has already developed. As a result, it appears that no new adhesions form more than seven days after an injury. Rather, the character of the adhesion changes, progressing from thin, filmy adhesions to more dense, vascular adhesions. The earlier in this process that adhesions can be removed, the less likely it is that they will recur and cause long-term problems.
Adhesion formation that occurs following surgery can be of two types; de novo adhesion formation or adhesion reformation. De novo adhesion formation means the formation of adhesions at a site that did not have any adhesions affecting it prior to surgery. This would include the formation of adhesions around the uterus following the removal of a fibroid tumor or the formation of adhesions around an ovary following removal of an ovarian cyst.
Adhesion reformation refers to the recurrence of adhesions following a procedure designed to remove pre-existing pelvic adhesions. This difference is important, as the techniques described below may be very effective at preventing de novo adhesion formation, while they appear to be somewhat less effective at preventing adhesion reformation
What types of surgeries can increase my risk of adhesions?
In most cases of adhesions, they form in the majority of women after gynaecologic pelvic surgery. Studies have shown that adhesions formed in 55-100% of patients who had reproductive pelvic surgery, whether open or laparoscopic.
For example:
• myomectomy (surgery to remove fibroids)
• tubal surgery (to remove an ectopic pregnancy)
• surgery on the ovary (to remove cysts)
• surgery for endometriosis
Even surgery to remove adhesions can lead to new adhesions. It can be a vicious cycle.
• Laparoscopic surgery (surgery done through several small incisions using a camera) has been known to cause less adhesion formation than laparotomy (surgery through one larger incision without use of a camera).
• Microsurgery (surgery using a microscope or magnifying glass, and special surgical technique) leads to less tissue damage and has a lower incidence of adhesion development than the traditional approach.
• Diagnostic procedures, which only involve a visual inspection of the organ(s), such as a diagnostic hysteroscopy or diagnostic laparoscopy, rarely lead to adhesions.
How can I reduce my risk of adhesions?
It starts with talking to your doctor and explaining your concerns about adhesions. There are techniques which can be used at the time of surgery to reduce the risk of developing adhesions. In addition to using microsurgery or laparoscopic techniques, prevention of infection is essential.
During surgery, various products are used to inhibit adhesion formation, known as adhesion barriers. These include gauze-like materials placed over the tissue which dissolve to become a gelatinous layer to reduce the incidence of post-operative adhesions. This material is eventually absorbed by the body.
Dr. Ruchi Tandon is a reputed Gynecologist practicing in leading hospitals in South Delhi namely Max and Apollo hospitals with over 14 years of experience in handling all kinds of Gynecological conditions including infertility and high risk Pregnancies.