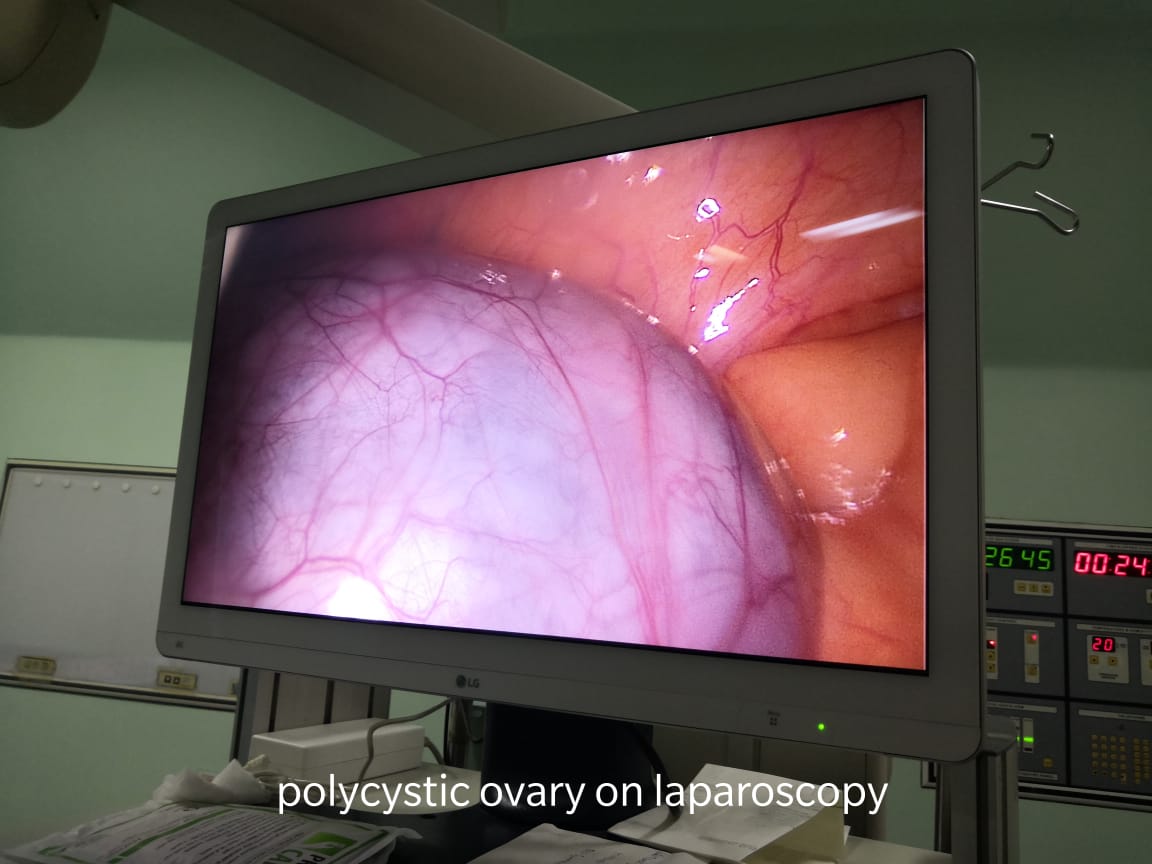
Polycystic ovary syndrome (PCOS) is a common condition that affects how a woman’s ovaries work.
The 3 main features of PCOS are:
- Irregular periods – which means your ovaries do not regularly release eggs (anovulation)
- excess androgen – high levels of “male” hormones in your body, which may cause physical signs such as excess facial or body hair
- polycystic ovaries – your ovaries become enlarged and contain many fluid-filled sacs (follicles) that surround the eggs (but despite the name, you do not actually have cysts if you have PCOS)
If you have at least 2 of these features, you may be diagnosed with PCOS.
What are polycystic ovaries?
Polycystic ovaries contain a large number of harmless follicles that are up to 8mm (approximately 0.3in) in size.
The follicles are under-developed sacs in which eggs develop. In PCOS, these sacs are often unable to release an egg, which means ovulation does not take place.
It’s difficult to know exactly how many women have PCOS, but it’s thought to be very common, affecting about 1 in every 5 women in the UK.
More than half of these women do not have any symptoms.
Symptoms of polycystic ovary syndrome (PCOS)
If you have symptoms of PCOS, they’ll usually become apparent during your late teens or early 20s.
They can include:
- irregular periods or absent periods
- difficulty getting pregnant as a result of irregular ovulation or failure to ovulate
- The excessive hair growth or hirsutism – usually on the face, chest, back or buttocks
- weight gain
- thinning hair and hair loss from the head
- oily skin or acne
PCOS is also associated with an increased risk of developing health problems in later life, such as type 2 diabetes and high cholesterol levels.
What causes polycystic ovary syndrome (PCOS)?
The exact cause of PCOS is unknown, but it often runs in families.
It’s related to abnormal hormone levels in the body, including high levels of insulin.
Insulin is a hormone that controls sugar levels in the body.
Many women with PCOS are resistant to the action of insulin in their bodies and produce higher levels of insulin to overcome this.
This contributes to the increased production and activity of hormones like testosterone.
Being overweight or obese also increases the amount of insulin your body produces.
What causes it?
Doctors don’t know exactly what causes PCOS. They believe that high levels of male hormones prevent the ovaries from producing hormones and making eggs normally.
Genes, insulin resistance, and inflammation have all been linked to excess androgen production.
Genes
Studies show that PCOS runs in families.
It’s likely that many genes — not just one — contribute to the condition.
Insulin resistance
Up to 70 percent of women with PCOS have insulin resistance, meaning that their cells can’t use insulin properly.
Insulin is a hormone the pancreas produces to help the body use sugar from foods for energy.
When cells can’t use insulin properly, the body’s demand for insulin increases. The pancreas makes more insulin to compensate. Extra insulin triggers the ovaries to produce more male hormones.
Obesity is a major cause of insulin resistance. Both obesity and insulin resistance can increase your risk for type 2 Diabetes.
Inflammation
Women with PCOS often have increased levels of inflammation in their bodies. Being overweight can also contribute to inflammation. Studies have linked excess inflammation to higher androgen levels.
How PCOS affects your body
Having higher-than-normal androgen levels can affect your fertility and other aspects of your health.
Infertility
To get pregnant, you have to ovulate. Women who don’t ovulate regularly don’t release as many eggs to be fertilized. PCOS is one of the leading causes of infertility in women.
Metabolic syndrome
Up to 80 percent of women with PCOS are overweight or obese. Both obesity and PCOS increase your risk for high blood sugar, high BP, low HDL (“good”) cholesterol, and high LDL (“bad”) cholesterol.
Together, these factors are called metabolic syndrome, and they increase the risk for heart disease, diabetes, stroke.
Sleep apnea
This condition causes repeated pauses in breathing during the night, which interrupts sleep.
Sleep apnea is more common in women who are overweight — especially if they also have PCOS. The risk for sleep apnea is 5 to 10 times higher in obese women with PCOS than in those without PCOS.
Endometrial cancer
During ovulation, the uterine lining sheds. If you don’t ovulate every month, the lining can build up.
A thickened uterine lining can increase your risk for endometrial cancer.
Depression
Both hormonal changes and symptoms like unwanted hair growth can negatively affect your emotions. Many with PCOS end up experiencing depression and anxiety.
Dr.Ruch Tandon, the Gynecologist, specializes in PCOS and is available at leading hospitals in South Delhi