What Are Fibroids?
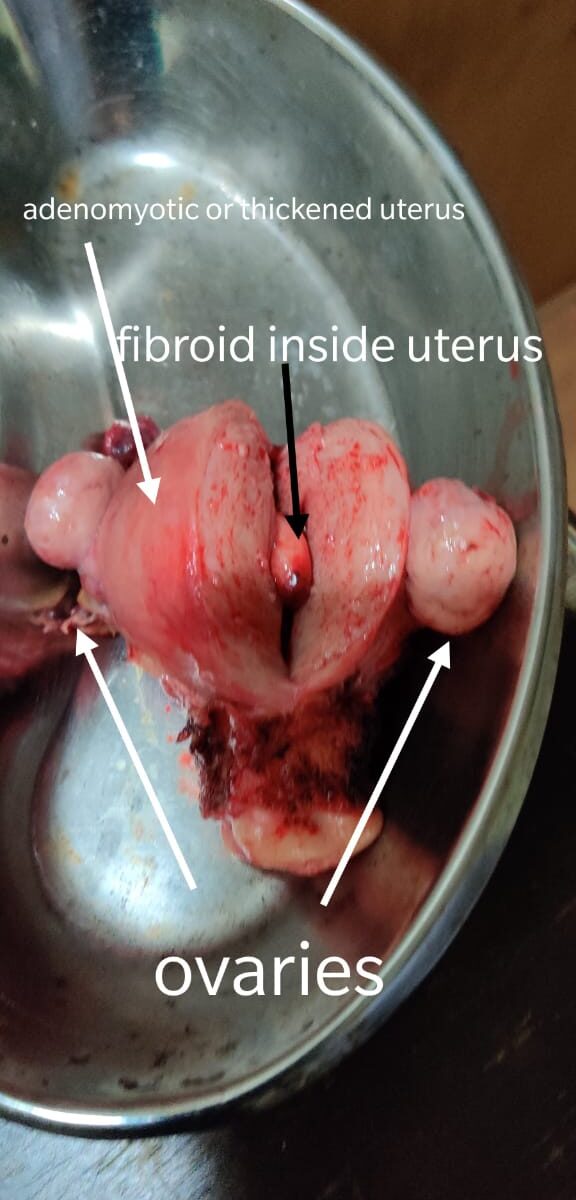
Fibroids, or leiomyomata (myomas), are common noncancerous growths that usually occur in or on the muscle walls of the uterus. One cell divides repeatedly and grows into a firm, rubbery mass separate from the rest of the uterine wall. Almost half of women older than 50 have these growths. They’re more common in African American women than in Caucasian women. They can grow as a single mass or more often as a number of masses of different sizes.
What Causes Fibroids?
The cause isn’t clear. Several factors probably work together to produce fibroids. These factors may be hormones such as estrogen, genetics (runs in families), and environmental. Being overweight, never having had a child, and getting periods before age 10 also may have an effect. The fibroids usually, but not always, shrink after menopause (change of life).
What Are the Symptoms of Fibroids?
Most fibroids (30% to 50%) cause no symptoms. Problems, when they occur, are related to the size and location of the fibroids. Fibroids may grow to be quite large so that a woman may look pregnant and have symptoms of pregnancy: pressure in the pelvic area (lower belly), heaviness, and need to go to the bathroom often to urinate. Fibroids in the uterine wall or in the cavity of the uterus may cause bleeding between periods or heavier and more painful periods. Constipation, backache, pain during sex, and lower belly pains may occur. Rarely, fibroids cause sudden pain or bleeding.
How Are Fibroids Diagnosed?
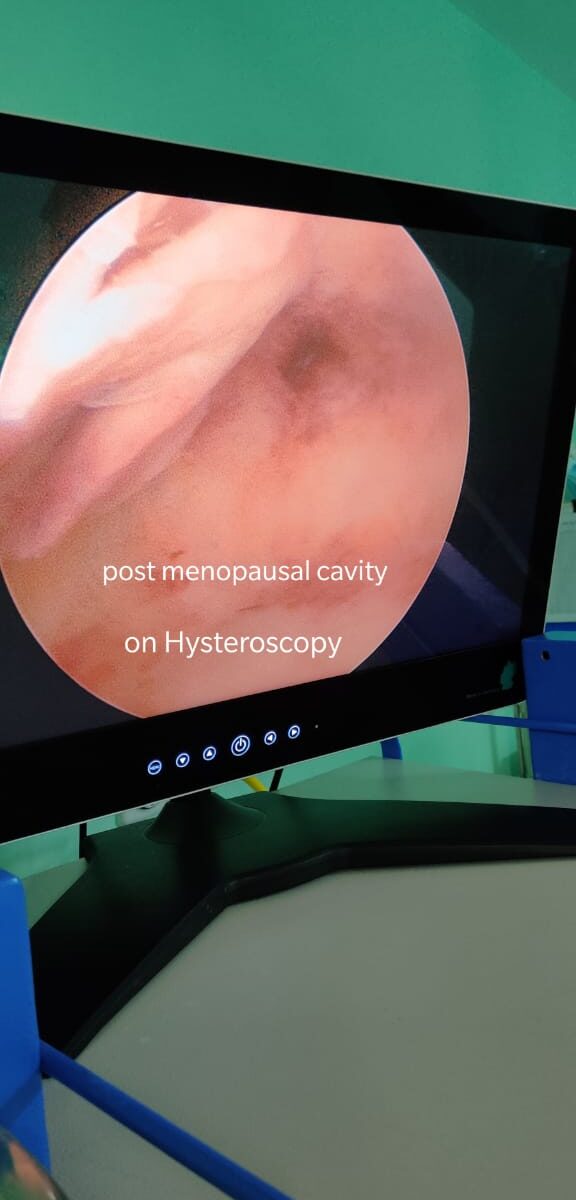
The health care provider will do an examination of the pelvic area. Ultrasound or x-rays may be used but aren’t always needed for diagnosis. The doctor may do a special procedure (hysteroscopy) for women with bleeding symptoms. This simple procedure lets the doctor look into the uterus to find the cause of the bleeding or to plan or carry out therapy.
How Are Fibroids Treated?
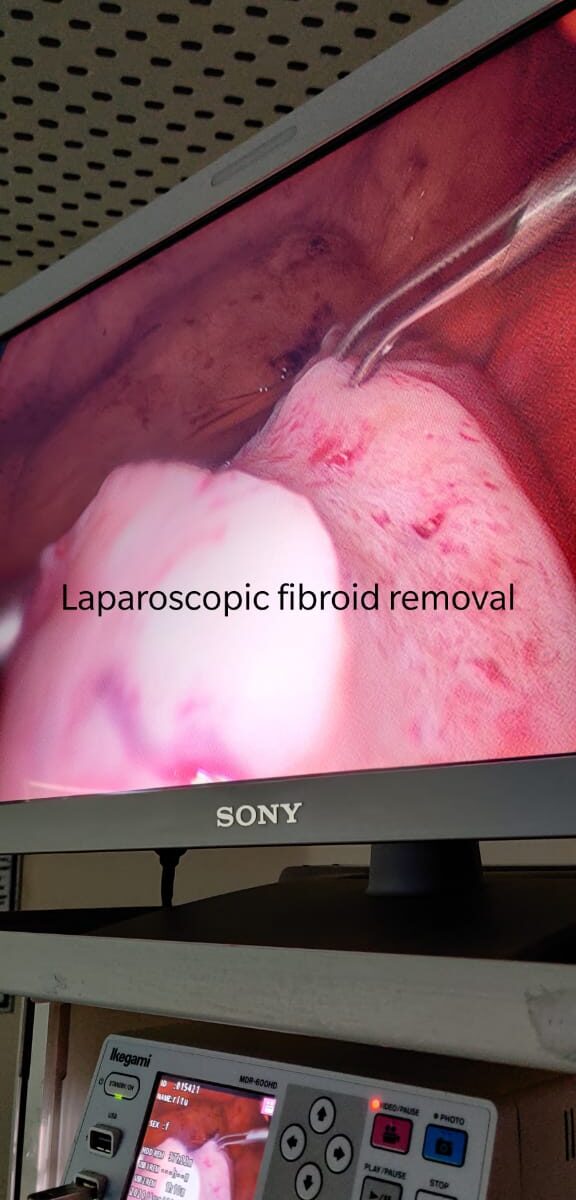
Most fibroids need no treatment and only regular checks to be sure that they’re not growing too large or causing problems. Medicines including hormones and drugs that act against hormones can be tried. If fibroids continue to be a problem, hysterectomy (surgery to remove the uterus) is an option. Sometimes, fibroids alone may be surgically removed (myomectomy), which saves the uterus if children are wanted. Another newer method is uterine artery embolization. In this method, arteries to the uterus are blocked so they don’t feed the fibroids. Myolysis (electric current destroys fibroids and shrinks blood vessels feeding them) and cryomyolysis (liquid nitrogen is used instead of electric current) are other methods. However, fibroids can return and mean more surgery later. Newer medicines may shrink fibroids, but this change is only temporary.
DOs and DON’Ts in Managing Fibroids:
• DO get regular health care provider checkups.
• DO tell your health care provider your concerns and describe your symptoms.
• DON’T delay having children just because you have fibroids. They usually won’t get in the way of pregnancy. If you do need treatment for fibroids, some treatments can temporarily or permanently prevent you from becoming pregnant.
• DON’T worry about getting cancer from fibroids. Typical fibroids are not cancerous.
Surgery for uterine fibroids
• Medication to treat fibroid symptoms usually only works while you are taking it. Many women who have severe pain and heavy menstrual bleeding end up considering surgery as an option. There are a number of different types of surgical treatments, each with its own pros and cons.
• Surgery is done in the hope that it can permanently stop the symptoms of uterine fibroids. Some women do, in fact, experience long-term relief. But surgery always carries risks too. Whether or not surgery is an option – and, if so, what kind of surgery – will depend on how the woman feels about the different advantages and disadvantages. The size, number and location of the fibroids will also influence the choice of treatment. Not all types of surgery are suitable for women who still want to have children.
• Your doctor may recommend taking hormones such as GnRH analogues several weeks before having surgery. These kinds of artificial hormones are used to shrink the fibroids. Doctors can then make smaller cuts during surgery, allowing the womb (uterus) to recover more quickly. The drug ulipristal acetate is sometimes used for this purpose too.
• But removing individual fibroids isn’t a good idea if it might cause too much scarring in the womb, or if the risk of bleeding during or after surgery is too high. Plus, it isn’t always absolutely certain that the symptoms will improve after surgery. Hysterectomy (surgical removal of the womb) is then an option – or possibly another non-surgical treatment approach such as uterine artery embolization (UAE, sometimes also called uterine artery embolization, or UFE). Uterine artery embolization cuts off the blood supply to the fibroid.
Dr.Ruchi Tandon is a Gynecologist practicing in leading hospitals in South Delhi namely Max and Apollo hospitals with over 14 years experience in handling all kinds of Gynecological conditions including Fibroids.