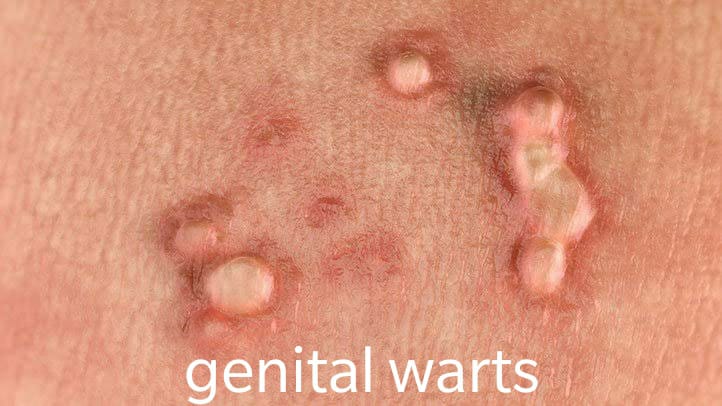
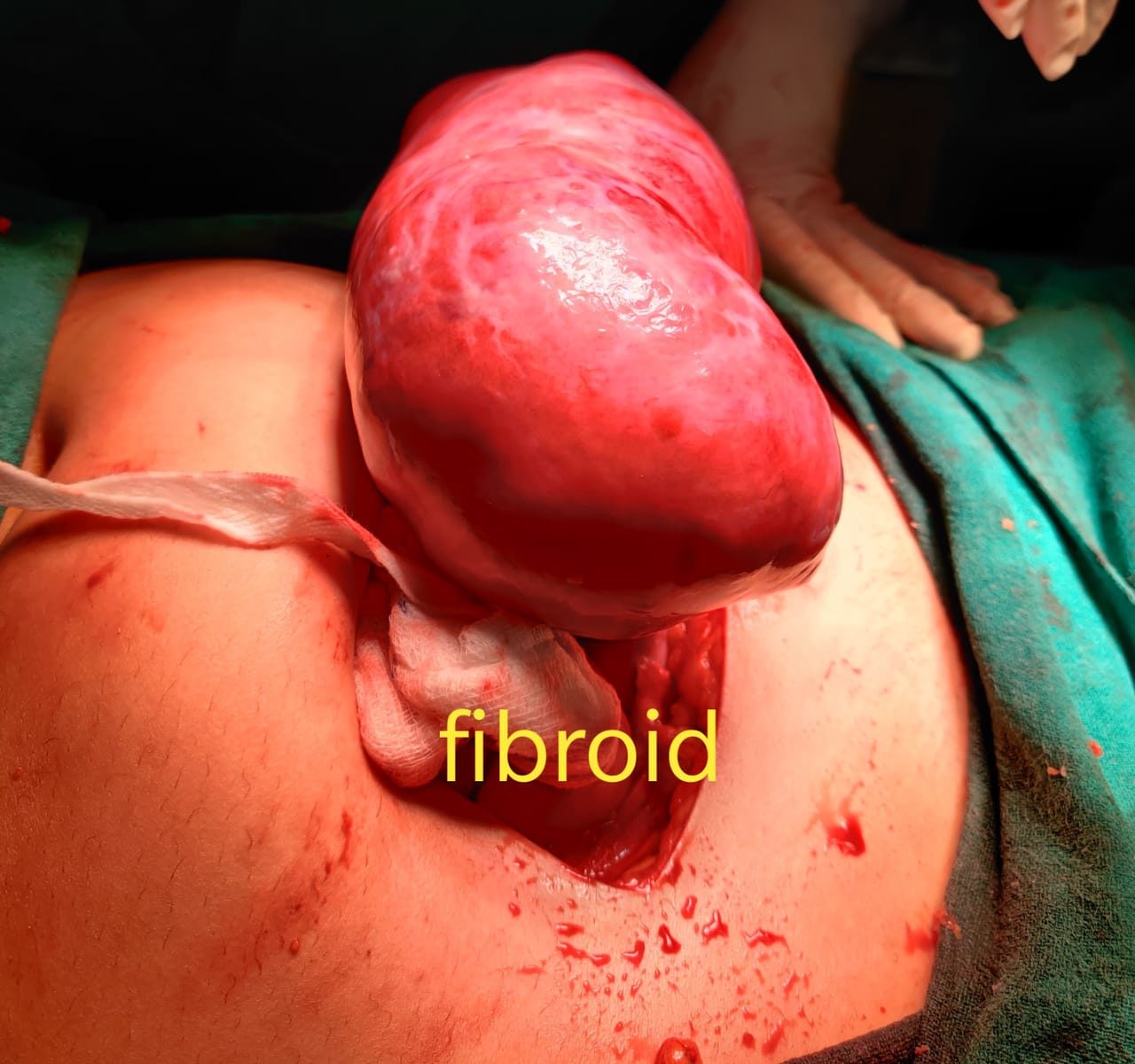
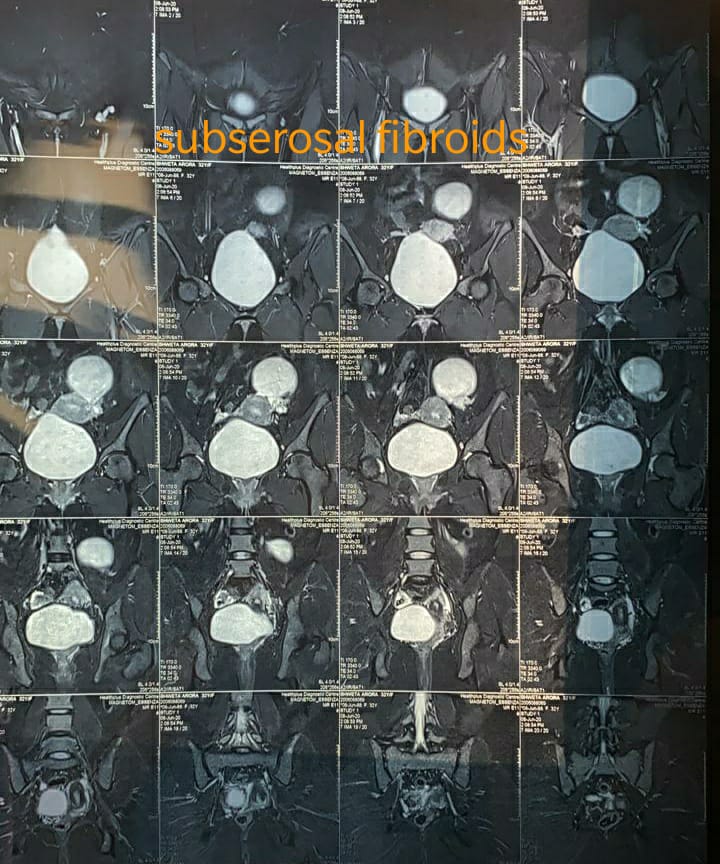
The vulva (Latin for womb or covering) consists of several layers that cover and protect the sexual organs and urinary opening. The fleshy outer lips of the vulva — the labia majora — are covered with pubic hair and contain fat that helps cushion the area. Inside the labia majora are the thinner, more pigmented and delicate flaps of skin called the labia minora. The labia minora join at the top to enclose the clitoris. The labia majora, labia minora, and clitoris are made up of erectile tissue, that is, tissue that can become engorged with blood.
The area between the labia minora, the vestibule, contains the openings to the urethra and the vagina, as well as the Bartholin’s glands, which are located on either side of the vaginal opening and produce lubricant for the vestibule. The flesh between the vaginal opening and the anus (not part of the vulva but often involved in vulvar skin problems) is the perineum. This is where the incision called an episiotomy is sometimes made during childbirth.
Getting a diagnosis for vulva skin conditionsVulvar skin conditions are highly treatable, but the treatment depends on the specific cause. And identifying the underlying diagnosis can be very challenging.
Tell your clinician about any other past or present medical conditions (including bladder and bowel issues) and any skin problems elsewhere on your body. For example, psoriasis anywhere on the body raises the risk of a vulvar condition known as lichen sclerosus. (This condition and others are described, below, in “Vulvar conditions and their treatment.”) Crohn’s disease, a chronic inflammatory intestinal disease, may cause abscesses or draining fistulas in the vulvar area, and vulvar skin problems are often one of its early symptoms. A mouth condition called lichen planus is another cause of vulvovaginal problems. (The term “lichen,” as applied to skin disorders, refers fancifully to skin lesions that resemble lichen on rocks.) Long-term treatment with oral steroids, immune suppressants, or antibiotics can affect vulvar skin and raise the risk infection.
Your clinician will want to know how you care for your vulvar skin, which can help identify possible sources of irritation. Even if you can’t pinpoint a change, that doesn’t mean your standard routine isn’t the culprit. Sometimes vulvar problems are the cumulative effect of long-term practices.
It’s often what you’ve done day after day, year after year, that causes the problem. If you wear abrasive clothing and engage in abrasive activities like bicycling or spinning class and wear tight workout clothes that expose your vulva to sweat or to detergent or soap residue, eventually it might catch up with you.
Report all the symptoms that concern you, including itching, burning, soreness, discharge, bumps, and any rashes the vulva. It will also help if you can provide a history of your symptoms and recall what seems to make them better or worse. Your clinician will examine the vulva, perhaps using a magnifying glass, and insert a speculum to inspect the vagina. She or he may test the pH (acid-base balance) of the vagina and take samples of secretions to examine under the microscope or culture for yeast. Remember, even if you’re seeing an experienced clinician, several visits may be needed to diagnose and improve certain vulvovaginal conditions.
The problem with self-treatment
When vaginal or vulvar itching occurs, women usually assume it’s a yeast infection and treat it with an over-the-counter antifungal cream. Often this does the trick, but not always. Instead, the cause of the symptoms might be dry skin, a sexually transmitted disease or bacterial infection, a less common strain of yeast that required special medication, or irritation by and allergic reactions to common products such as soaps, creams, and lotions.
If yeast isn’t the problem, an antifungal cream isn’t the solution. And if your skin is already irritated, you may exacerbate the problem by introducing preservatives (such as alcohol or propylene glycol) and other ingredients contained in many antifungal remedies. That’s why it’s important to see your gynecologist or dermatologist if a problem persists after you’ve tried a standard antifungal cream.
Another common response of women faced with a vaginal discharge or itch is to wash the vulvar skin vigorously, on the assumption that this will disinfect the area or remove irritants. But aggressive cleansing can add to the irritation. Until the problem is diagnosed, it’s best to follow a gentle skin care routine (see “Gentle vulvar care”). In fact, gentle cleansing applies whether you have a vulvar skin condition or not: Wash the area gently with your fingertips or a soft cloth and pat dry with a soft towel. Don’t use a rough washcloth, and don’t rub.
Vulvar skin conditions and their treatment
Several vulvar skin conditions are familiar from other areas of the body but may be difficult to recognize when they appear on the vulva. These include the following:
Eczema. This inflammatory skin condition disrupts the skin’s surface, causing red patches and thin cracks, weeping, and crust formation. On the vulva, crusts are less likely, but eczema may initiate a cycle of vulvar itching and scratching that leads to lichen simplex chronicus — thickened and intensely itchy skin. If eczema affects an area of the vulva called the vestibule, it may cause stinging and burning. Sometimes eczema appears in early childhood and its cause is unknown. More often, it begins with exposure to an irritant or allergen (see “How irritating”).
To diagnose vulvar ecz
Many things can cause an allergic reaction or irritate vulvar skin. Here are some of the leading suspects:
Irritants (on exposure, can cause immediate stinging or burning)
- Soap, bubble baths and salts, detergent, shampoo, conditioner
Adult or baby wipes
Panty liners and their adhesives
Nylon underwear, chemically treated clothing
Vaginal secretions, sweat, and urine
Douches, yogurt
Spermicides, lubricants
Perfume, talcum powder, deodorants
Alcohol and astringents
Allergens (symptoms may not appear until several days after exposure)
- Benzocaine
Neomycin
Chlorhexidine (in K-Y Jelly)
Imidazole antifungal
Propylene glycol (a preservative used in many products)
Fragrances
Tea tree oil
Latex (in condoms and diaphragms)
Adapted from The V Book, by Elizabeth G. Stewart, M.D., and Paula Spencer (Bantam Books, 2002).
ema, the clinician will ask about your symptoms; your history of eczema, allergy, and related conditions; your vulvar cleansing habits; and any products the vulva has been exposed to. During the exam, she or he will look for redness, scaling, cracking, and thickening.
All eczema requires gentle skin care. In simple cases, patients use topical corticosteroid ointments twice a day for two to four weeks and then gradually reduce the frequency until the symptoms are gone. Severe cases may require a short course of a potent corticosteroid ointment.
During treatment, you must stop scratching, so your clinician may prescribe an antihistamine (usually taken at night to prevent daytime drowsiness). A cold pack can also help relieve itching.
Dr. Ruchi Tandon is a Gynecologist, practicing in leading hospitals in South Delhi namely, Max Smart superspeciality hospital, saket and Apollo hospitals. She has experience of over 13 years in handling all vulval skin lesions.